

Kajiado County, Kenya, August 30, 2023 – Patients living in Kenya’s Kajiado County and surrounding areas will have access to comprehensive eye health care, thanks to a new eye unit now open in the community.
The Kajiado County Referral Hospital Eye Unit was established in partnership by Operation Eyesight Universal with the County Department of Health and constructed in partnership with CBM Christian Blind Mission. Equipped with state-of-the-art diagnostic and surgical equipment, the new facility can provide a range of eye health services, including comprehensive eye exams and prescription eyeglasses fittings to diagnoses and sight-restoring eye surgery.
“Healthy eyes open up a future full of possibility and opportunity for individuals and entire communities,” says Alice Mwangi, Operation Eyesight’s Country Director for Kenya. “We are bringing quality eye health care to people’s front doors, and this new eye unit will serve as a hub for the entire community, connecting people with not only eye health care but also their local health system.”

The new eye unit was constructed as part of the Vision Impact Project, a four-year project started in October 2021 that aims to bring eye health care to unreached communities in Kajiado County, where blinding trachoma is endemic and other leading causes of vision loss include uncorrected refractive error and cataract. The project will train a local team of 23 local eye care workers and 175 eye screeners to use Peek Vision’s mobile app for screening and referrals. They will screen nearly 720,000 residents through door-to-door outreach. The project will also train 140 healthcare providers in primary eye care.
“Trachoma and other eye diseases such as cataract and untreated refractive error have had a devastating impact on many patients and families in the area, and many have faced barriers to accessing eye health care, including cost and lack of locally-available services,” explains Mwangi. “Today, we are able to better meet demand while also raising awareness about the eye health services that are now available, through education in the surrounding community.”
Since the project launched, Operation Eyesight has trained 33 local community health volunteers to deliver health education, screen community members for eye problems and refer them for treatment if needed. So far, 199,894 people have been screened for eye conditions and over 21,822 people have received treatment, including more than 5,125 people who have received prescription eyeglasses and 183 people who received sight-restoring cataract surgery.
“This is about taking a collaborative approach to care. It starts with outreach in the community and connecting patients and families with comprehensive eye care through this new eye unit,” says Dr. Ritu Ghosh, Operation Eyesight’s Global Director, International Programmes. “Together with the community and local leaders, we are not only transforming eye health care in the region but also strengthening the entire health system.”

To date, Operation Eyesight and partners have declared 35 villages in Kenya as avoidable blindness-free, which means the communities are free of any untreated cases of vision loss.
Operation Eyesight is a Canada-based international development organization working to prevent blindness and restore sight in sub-Saharan Africa and South Asia. In 2023, Operation Eyesight is celebrating 60 years of collaborating with local hospitals and government partners to invest in sustainable eye health treatment, blindness prevention and community development. Operation Eyesight is implementing projects in eight counties in Kenya: Kajiado, Elgeyo Marakwet, Nandi, Kisii, Narok, Transnzoia, Uasin-Gishu and West Pokot.
-30-
For further information please contact:
Colin Zak
Communications Specialist
Operation Eyesight Universal
Zakc [at] operationeyesight.com
@OpEyesight
July 12, 2022 – Kenya and Tanzania are one step closer to eliminating blinding trachoma, as the two countries today launched a cross-border mass drug administration exercise.
The joint effort, led by Operation Eyesight in partnership with the ministries of health in both countries, as well as Sightsavers, will distribute antibiotics to more than 1.3 million people with trachoma or at risk of developing the painful bacterial infection. This will provide much-needed treatment to communities living along the Kenya-Tanzania border, across the counties of Kajiado, and Narok on the Kenyan side and the neighbouring districts of Ngorongoro and Longido on Tanzanian side.

In Kenya, trachoma is endemic in 12 counties, impacting a combined population of approximately 11 million people. If left untreated, this painful bacterial infection leads to irreversible blindness.
“Trachoma knows no borders, and many pastoralist communities in the area are semi-nomadic. Therefore, collaboration between governments is critical to ensure no patient at risk is unable to receive antibiotics,” explains Alice Mwangi, Operation Eyesight’s Country Director for Kenya. “Antibiotics are an effective and proven way to prevent the spread of trachoma. Together, we are eliminating trachoma from entire villages and communities.”

Teams of government health workers and partners like Operation Eyesight will begin efforts in Narok and coordinate work with teams in nearby Tanzania.
Mwangi says the upcoming Mass Drug Administration (MDA) builds on the success of the previous MDA in Narok County, which provided antibiotics to 460,000 people needing treatment last year. Previous efforts by both governments to distribute antibiotics saw sections of the local communities miss out on treatment as they moved in search of pasture.
“Collaboration with both ministries of health is a historic step towards eliminating trachoma from Kenya for good,” Mwangi adds.
We are partnering with national and county governments with the shared goal of eliminating trachoma from Kenya by 2025.
SAFE from trachoma
Although it can be treated with a simple dose of antibiotics, more than 1.9 million Kenyans and 116 million people across Africa are in immediate need of treatment of blinding trachoma. This bacterial infection causes the eyelashes to turn inwards, causing painful scarring on the cornea, leading to permanent blindness if left untreated.
Because trachoma is spread through flies and personal contact, women and children are most at risk of contracting or re-contracting this blinding condition.
Distributing antibiotics is just one part of the World Health Organization’s ‘SAFE’ strategy for eliminating trachoma:
“Eliminating trachoma goes beyond simply treating the disease. It’s also about issues like access to water and sanitation and bringing health education to communities. This plays an integral role in preventing re-transmission of the disease,” explains Mwangi.
“Community eye health activities like these are helping us shift the dial on not only trachoma, but other conditions as well.”
Neglected Tropical Diseases: diseases of poverty and inequality
Trachoma is one of 20 diseases classified as a Neglected Tropical Disease (NTD) – a group of diseases that have one thing in common: they debilitate and disfigure.
They also affect one billion people living in poverty worldwide.
Operation Eyesight is inviting governments, institutions and organizations globally to join us in signing the Kigali Declaration – a pledge to partner together to ensure that trachoma and other NTDs are eradicated, eliminated or controlled by 2030.
“Ending Neglected Tropical Diseases at its core is about addressing the root causes of these conditions – poverty and inequality. That’s why Operation Eyesight endorses the Kigali Declaration,” says Kashinath Bhoosnurmath, President and CEO of Operation Eyesight.
“As we move globally towards achieving universal health coverage and achieving the UN’s Sustainable Development Goals, we see each one of these are also steps towards ending needless vision loss.”
Bhoosnurmath says the Kigali Declaration is not just about eliminating trachoma and other NTDs, but also about taking steps to address inequality, strengthen health systems and leverage the unique strengths of communities.
“We hope that by signing this joint declaration, we can build on our success to date and take more steps forward as a global community.”

Making strides
Mwangi says the number of active trachoma cases in the region has steadily decreased due to the efforts of Operation Eyesight, governments and other partners. Rates of infection have steadily decreased from 2004 when trachoma infection rates in endemic areas of Kenya were above 30 per cent, to between 12.6 and 19.8 per cent in 2018.
The Kigali Declaration invites us all to a shared commitment to achieve the UN’s Sustainable Development Goals that target NTDs over the next decade.
“We have made great strides in eliminating trachoma from entire regions,” adds Mwangi. “But more work needs to be done in Africa in particular.”
Donate today to help prevent blindness and restore sight.
Nairobi, Kenya, September 10, 2021 – Today, September 10, Operation Eyesight Universal and the Uasin Gishu County Government officially launched their School Eye Health Program in the county. Through support from the United States Agency for International Development (USAID) Child Blindness Program, the two-year program will provide vision screening and treatment for 80,000 children and 3,000 teachers in the sub-counties of Soy, Turbo and Aynaoui. (Video of the launch event here.)
“Access to eye care for school-age children is critical; about 80 percent of what a child learns is processed through the visual system,” said H. E. Governor Jackson Mandago, Uasin Gishu County. “This program will ensure that children receive the eye care they need, so they can continue to learn and achieve their dreams.”
While the official launch takes place today, program implementation began in March 2021 with 20 teachers being trained to use the Peek Acuity app, developed by Peek Vision, to identify students with eyesight problems. As of August 20, more than 27,000 children have been screened and 2,242 students have been referred for treatment. (Read Rehema’s story here.)
Eye screenings will be conducted in 200 schools over the course of two years. Students in need of eye care will be referred to a mobile ophthalmic triage team or the nearest eye health facility, and transportation will be provided as needed.
Essilor East Africa is supplying the prescription eyeglasses to correct the vision of children (and teachers) with refractive error. Children requiring further care, such as cataract surgery, will be referred to the Huruma Sub-County Hospital Eye Unit or one of Operation Eyesight’s partner hospitals for treatment. All students will receive the same level of quality care, regardless of their gender, treatment location or ability to pay.
“By investing in children’s eye health to treat diseases, correct refractive error and restore sight, we can transform lives, families and communities,” says Alice Mwangi, Country Manager – Kenya, Operation Eyesight. “We know that women and girls are more likely to suffer from vision impairment and less likely than men and boys to receive treatment and care. Through this project, many of the barriers faced by girls, such as cost and lack of transportation, are addressed. We will educate teachers, parents, grandparents and health workers on the additional barriers faced by girls so they understand and can play a role in addressing these challenges.”
In addition to providing screenings and treatment, the program will provide eye health education for students and teachers and encourage proper hand and face washing to prevent the spread of blinding trachoma. Eco-Soap Bank, a collaborating partner, is providing 100,000 bars of soap for children and teachers to use at school and at home. Operation Eyesight conducted a similar school screening program in Trans Nzoia County from 2016 to 2018 with great success. The program in Uasin Gishu County builds on the lessons learned and aims to not only provide quality eye health services to students but to further refine the program model for scaling up in Kenya. Program results will be shared at the county, national and international levels, enabling other organizations to use these findings when developing their school screening programs.
Operation Eyesight is working in partnership with the Ministries of Health and Education to integrate eye health care into the primary health and education systems and ensure the sustainability of eye health care services.


For more information, contact:
Elizabeth Roden
Director, Marketing & Communications
RodenE[at]operationeyesight.com
About Operation Eyesight Universal
Operation Eyesight is a Canada-based international development organization dedicated to eliminating avoidable blindness in developing countries. It was founded in 1963, and today works in Ethiopia, Ghana, Kenya, Liberia, Zambia, Bangladesh, India and Nepal to prevent blindness and restore sight. Operation Eyesight invests in sustainable treatment, prevention and community development activities to address specific eye health problems as well as the root causes of blindness. To learn more, visit operationeyesight.com.
About Peek Vision
Peek Vision powers eye health organizations with a proven suite of solutions to expedite delivery of care. The result is that more people can get the treatment they need. Peek works in low- and middle-income countries, partnering with health providers, NGOs and governments. With Peek, partners gain better insights, increase efficiency and deliver stronger health systems. Peek’s vision is to bring better vision and health to everybody.
This media release is made possible by the generous support of the American people through the United States Agency for International Development (USAID). The contents are the responsibility of Operation Eyesight Canada and do not necessarily reflect the views of USAID or the United States Government.
For most of her life, Napolo from Narok County, Kenya suffered from eye pain. The 78-year-old first noticed the discomfort when she was in her thirties. She said it felt like there was always sand in her eyes.
Then her eyelids started turning inwards, causing more pain and irritation. She tried traditional remedies like plucking her eyelashes, but nothing helped. Her vision worsened over time.
One day, a community health worker came to Napolo’s doorstep to check on the family’s vision. Thanks to the primary eye care training we’d provided, the community health worker took one look at Napolo’s eyes and instantly knew what the problem was – a trachoma infection.
Trachoma is a bacterial eye disease that is a leading cause of blindness in areas with water shortages and crowded living conditions. The infection spreads easily through hands and clothing, and also through direct transmission by flies. If left untreated, trachoma forces the eyelid inward – like Napolo’s – making the eyelashes rub painfully against the cornea. Over years, it can lead to permanent scarring and irreversible vision loss.
The community health worker helped connect Napolo to our partner hospital for treatment. As Napolo was in the late stage of the disease, she required surgery. At our partner facility, the Talek Health Centre, she underwent an operation that corrected her inward-turned eyelids. The procedure brought her immense relief and preserved her remaining vision.
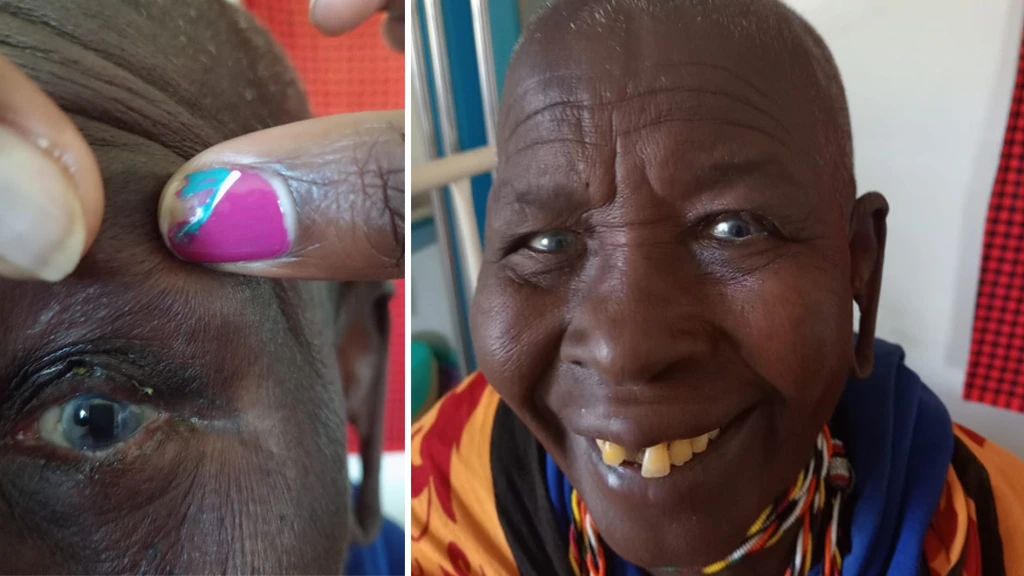
Stories like Napolo’s are an example of how we strive to address the root causes of avoidable blindness through a disease control approach. Our model helps us diagnose, treat and prevent the major causes of vision loss, including cataract, diabetic retinopathy, glaucoma, trachoma and uncorrected refractive error.
Throughout Kenya, Ethiopia and Zambia, we’ve been working with communities and partners to eliminate trachoma through a four-step approach known as SAFE.
The SAFE acronym stands for:
In Kenya, we work with government partners to distribute antibiotics to regions where trachoma is endemic. These antibiotics help prevent infection and can help clear up existing infections.

And because trachoma spreads quickly in areas where water is scarce, part of our approach is to make sure that people in our partner communities have access to a clean water source – by repairing and drilling water boreholes.
In the past couple years, we’ve focussed on training groups of local volunteers – called “Area Pump Minders” – in hand pump maintenance. That way, when a village borehole breaks down, someone in a nearby community will be around to fix it quickly. Throughout 2024, we hired on some of the Area Pump Minders we’d already trained to repair 129 boreholes – benefiting the nearly 130,000 thousand community members who depend on them.
Glaucoma is a tricky condition that often goes unnoticed until the damage is already done. Caused by increased pressure within the eye, it affects the optic nerve at the back of the eye, resulting in loss of nerve function and peripheral vision.
This often occurs painlessly, making it hard to detect. And any vision loss caused is generally considered irreversible. But if glaucoma is diagnosed early enough, it can be treated and managed with eye drops and medication, as well as regular checkups.
Ayetu, a farmer in Ghana’s Central Region, first noticed that he was having problems with his vision several years ago. After visiting the hospital, where he got a diagnosis of glaucoma, he started using eye drops. But finances were tight, and he found it difficult to pay for the medicine and attend his monthly appointments. Eventually he gave up and turned to herbal remedies, and when he did, his vision worsened.

In 2022, we started a community health project with the Winneba Municipal Hospital. Glaucoma patients with financial difficulties, like Ayetu, were told that their medication and appointments would be given free of charge – thanks to the generosity of donors.
When Ayetu found out he could get his medication once again, he felt enormous relief. He had worried about going totally blind, leaving his 75-year-old wife to manage the household on her own. Now, he says that the pain and tearing in his eyes has ceased, and the pressure has stabilized. “I was overwhelmed with gratitude when I started receiving these medications every month,” he says.
Today, little Ayan and Vyan in India have a bright future ahead of them – but as infants, these twin girls narrowly escaped a life of blindness.
Born two months early in June 2022, the girls weighed just three pounds each and suffered from lung infections. They were rushed to a nearby Neonatal Intensive Care Unit (NICU) in their city of Moradabad where they were stabilized. While there, the doctor treating the girls recommended that they undergo screening for Retinopathy of Prematurity, also known as ROP.
Retinopathy of Prematurity, as the name suggests, is a condition that can occur in preterm and low-birth-weight babies. It causes abnormal growth of the blood vessels that attach to the retina, which leads to later vision loss if left untreated. It’s difficult to detect, and in the worst case scenario it can cause a child to go suddenly, irreversibly blind.
Since 2022, we’ve been working closely with our partners at the C. L. Gupta Eye Institute to screen and treat preterm infants throughout Moradabad and its surrounding districts for ROP. The Retinopathy of Prematurity Eradication Project runs a fully-equipped mobile screening van. A highly trained optometrist makes rounds of all the local NICUs, screening babies for ROP, treating simple cases and referring more complex cases back to the base hospital.

Little Ayan and Vyan underwent screening, and both were diagnosed with severe ROP. At just five weeks old, they underwent eye injections, followed by laser treatment. Now, thanks to regular checkups, their condition has been addressed, and the little girls can live up to their full potential with their vision intact.
These twin girls are just two of many infants that have benefited from increased ROP screening in their community. In 2024, we expanded the program to 28 NICUs in five districts across the region, enabling us to screen an additional 1,500 infants for ROP and provide treatment for 400 of them.
At just eight years old, Fassikaw in Bahir Dar, Ethiopia decided he’d had enough of school. His eyes were always watery, he couldn’t read the blackboard, he had to hold books just inches from his face and his grades were suffering as a result. He told his parents he wanted to quit.
His parents didn’t let him leave school, and when they heard about a school eye health program that was offering free diagnosis and eyeglasses to students, they jumped at the chance. They took Fassikaw to our partner hospital where they learned that he needed strong corrective glasses. Thanks to Partners in Education Ethiopia and our generous donors, he received the eyeglasses at no cost. Now that he can see, Fassikaw is finding school much more engaging, and his grades are on the rise.

What the little boy probably doesn’t know is that vision impairment like his prevents a lot of children around the world from finishing their schooling. In fact, children with vision loss are up to five times less likely to be enrolled in formal education in low-and middle-income countries, and a pair of glasses can reduce the odds of failing a class by as much as 44 per cent.
That’s why we help run school eye health programs, reaching children right where they need vision care the most – in the classroom. By training teachers and school health coordinators in primary eye care, we’re able to screen thousands of students in just days, quickly identifying those with possible vision loss for further referral. That way we can help more students like Fassikaw stay in school and thrive in life.
Adults, of course, also suffer from refractive errors, and sometimes providing a pair of reading glasses or prescription eyeglasses can change the course for an entire family. Take Junmoni’s story as an example. The mother of two in India helped support her family’s income by doing handloom weaving from her home. But as she got into her forties, she found it harder and harder to see the intricate patterns she was weaving. In despair, she was readying herself to sell off her handloom when she was surprised one day by a knock on the door. A visiting community health worker did a quick vision screening test and told Junmoni she likely just needed a pair of glasses. With a referral in hand, Junmoni visited one of our eye screening camps where she got a diagnosis and a pair of prescription bifocals all free of charge. Now she’s weaving again and saving up so she can send her young daughter to college.

We can provide eyeglasses to people like Junmoni and Fassikaw, with all associated expenses, for about $20 dollars apiece. In 2024, we distributed more than 270,000 pairs of eyeglasses – that’s a lot of lives transformed.
Across the world, more than 17 million people are blind due to cataracts, and cataracts cause another 34 million people moderate to severe vision impairment. But they are easily treated. A simple day surgery, one per eye – at the cost of about $75 Canadian dollars – can restore vision.
Despite that, millions around the world aren’t getting the surgery they need. The barriers are innumerable but usually include lack of financial resources to pay for the surgery, and lack of transportation to access the healthcare system. That’s why we work in rural, remote and underserved communities, identifying eye conditions like cataracts on people’s doorsteps and connecting them to the healthcare system – then ensuring that their treatments and transportation are subsidized or provided free of charge.
For someone like 85-year-old Esther in Kenya, a visit from a community health promoter made all the difference. Living in the remote village of Sitet, Esther struggled to get together the money just to visit the nearest hospital, let alone pay for the appointment.
About 10 years ago, when Esther was chopping wood, a log bounced up and hit her in the left eye. The pain was extreme, but she decided to wait and see what happened. A week later, in unbearable pain, she travelled to the hospital for help. There she received pain medication and a referral to an eye hospital. But by then, she was out of money. She went home and the vision in her left eye never recovered.
Three years ago, she started to notice the vision in her right eye was also fading. Soon, she could no longer manage her household, and her daughter had to move in with her.
“She had to leave her home to stay with me and help,” says Esther, about her daughter. “At some point, I just wanted to die… I didn’t want to hold her back from her life.”

One day, hope arrived in the form of a community health promoter who knocked on Esther’s door. The health promoter referred her to an eye screening camp, where she was diagnosed and referred for cataract surgery on her right eye. Unfortunately, the damage to her left eye was irreversible, making treatment of her right eye even more essential. As part of our program, Esther’s transportation, appointments and surgeries were all paid for, thanks to the generosity of our donors and partner, Johnson & Johnson.
Today, Esther is back to living independently – visiting friends, walking to church and picking and drying her own coffee beans.
Every year, the community health workers we train bring hope to thousands of seniors like Esther who once believed blindness was inevitable. In 2024 alone, community health workers helped us restore sight by making referrals for more than 230,000 cataract surgeries – giving people back their independence and dignity.
Seeing care through to the end
Our model offers patients the full continuum of care – from screening and diagnosis, through treatment, to follow-up. After surgery, our teams make home visits to check on healing, answer questions and make sure patients attend follow-up appointments. This helps us troubleshoot issues early and keep recovery on track.
For cataract patients, follow-up is especially important. When someone has cataracts in both eyes, we often schedule surgeries several weeks apart. That gap gives time for healing and reassessment, because the outcome of the first surgery can guide the second.
Eye surgery changes lives, but recovery looks different for everyone. By staying with patients through every step, we prevent complications, improve outcomes and build trust. When communities know we’re here for the long haul it makes our work more sustainable, with healthier futures for all.
Vision loss doesn’t have to be inevitable. From Napolo in Kenya to Ayetu in Ghana and little Ayan and Vyan in India, these stories remind us that blindness can often be prevented or treated when care is accessible. Through community outreach, early diagnosis and partnerships that remove the financial and geographic barriers, we’re restoring sight and transforming lives. But the need is still great. Millions of people remain at risk simply because they lack access to basic eye care. Together – with continued support and collaboration – we can ensure that no one is left in the dark. Donate today to help us in our mission to prevent blindness and restore sight.
If you sprain an ankle or come down with a bad cough, your first stop is usually your family doctor. But when it comes to blurry vision, the path to care often looks very different. Around the world, eye health is still treated separately from primary health care, creating gaps that leave people without the vision help they need. Even in countries with universal health coverage, you might receive a complex eye surgery at no cost, yet pay out of pocket – or use private health insurance – for something as simple as a pair of eyeglasses.
At Operation Eyesight, we believe this needs to change. That’s why we’re working to strengthen areas of overlap between primary eye care and primary health care in our countries of operation. That means supporting the World Health Assembly’s integrated people-centred eye care (IPEC) resolution by working to integrate eye health into national health systems – and increasing access to free or subsidized eye health care.
It also means addressing the root causes of avoidable vision loss. In some regions in Africa, we bring fresh water and hygiene education to communities to help prevent infectious eye conditions. We also work to make sure our services offer more than just eye care, but can also link patients to other types of health care.
Health conditions rarely exist in silos – and vision loss is no exception. Diabetes, for example, increases the risk of eye conditions like cataracts. For 15-year-old Vanessa in Zambia, blurry vision was one of the first signs of the disease. When she started having problems reading the blackboard at school, a teacher sent her to our vision centre in her community of Matero for a checkup. From there, she received a referral to our partner hospital, where she learned that she not only had cataracts, but diabetes as well. Doctors helped her get her blood sugar levels under control, and then she got cataract surgery. Today, she is managing her diabetes and thriving in school, with dreams of becoming a doctor.

Vision problems can also cause a downward mental health spiral. Benson, a farmer in Kenya, lost his ability to work due to poor vision. As a result, he became angry and depressed, then turned to alcohol and drugs to cope with his situation. Luckily, his family got him into a drug and alcohol rehabilitation facility, where a visiting doctor diagnosed him with cataracts. Benson underwent surgery on both eyes, provided free of charge thanks to the support of our donors, and can see clearly now. Buoyed by his miraculous recovery, Benson finished up his time at the rehabilitation facility and happily threw himself back into farming.
In Canada, where Operation Eyesight is based, navigating eye care can be confusing. While the Canada Health Act covers medically-necessary eye health services, routine vision care like eye exams and prescription glasses often isn’t part of the deal. That leaves provinces and territories to fill in the gaps, and the result is a patchwork system. For example, seniors in Ontario get routine eye exams covered once they hit 65, but in Newfoundland and Labrador, those same seniors might have to pay out-of-pocket. It’s inconsistent, and it’s especially tough on vulnerable populations.
There is some support through the Federal Non-Insured Health Benefits (NIHB) program, which covers eye exams and eyewear for eligible First Nations and Inuit individuals. But even that has its hurdles: remote communities, limited healthcare infrastructure and cultural differences that make accessing care more complicated than it should be.

The passage of the National Strategy for Eye Care Act in 2024 was a major step forward in addressing these issues. As chair of the Canadian Eye Health Coalition, Operation Eyesight is helping shape a national framework that prioritizes equitable access to vision care. Our Global Director of International Programs, Kris Kelm, explains why it’s important that we have a seat at the table during the consultation period and beyond.
“We know that there will be many voices in this conversation with diverse interests, and we want to ensure there is representation from patients who have the least means and the least ability to access vision care,” he says. “The fact that we have over 60 years of experience working in this sector gives us a strong background to speak credibly to how we need to approach things in Canada, and our community partners can provide valuable insights to help shape eye care for all.”
He adds that Canada can learn from some of our countries of work, where eye health has been better integrated into the overall health systems and other public frameworks. As an example, he points to Ghana, where we work with the ministries of health and education to screen and treat students for eye conditions in the public school system. We have similar programs in Kenya and Zambia, too.
Another example is in India, where we are working with state governments to establish vision services in pre-existing government health centres. Building the capacity of vision care facilities within the country’s national health care system ensures that services reach the most underserved populations, as patients who are able to pay most typically seek care at for-profit facilities, rather than attending government services.
Shakuntala, in Madhya Pradesh, India, spends her days walking door to door through villages in her region, checking in on the health and well-being of families. She’s one of the million-strong network of Accredited Social Health Activists (ASHAs), employed by the Indian government, who deliver primary health care at the community level.

Her work includes providing pregnancy advice, supporting newborn care, educating parents about vaccinations and vitamins for children, and making all kinds of referrals to local clinics and hospitals. In 2022, Shakuntala added another set of skills to her toolkit: conducting primary eye health screenings, thanks to training provided by our Operation Eyesight team, in partnership with the Government of Madhya Pradesh. Shakuntala learned to measure visual acuity using an eye chart. She also learned to identify the signs and symptoms of various eye conditions. Once she identifies a patient with a possible eye condition, she refers them to the base hospital for diagnosis and treatment. In the meantime, she continues to provide advice and referrals on nutrition, vaccinations, prenatal care and other health concerns.
Shakuntala is just one of the thousands of community health workers we work with across the globe. In all our countries of work, we partner with existing health systems to recruit community health workers, mostly women, to help us deliver our programs. The health workers develop strong ties within the communities, resulting in high acceptance and trust in our programming.

Mabel, a community health nurse in Ghana, was trained in primary eye care so that she could identify eye health issues in addition to her regular duties. She says that being able to screen people at their home allows her to reach many women and girls who probably wouldn’t have left the village to seek eye health care, due to household responsibilities.
Anyone who has had a case of pink eye knows that having red, inflamed and itchy eyes isn’t much fun. But in some parts of the world, an eye infection can be a much more serious problem. Trachoma is an infectious eye disease that leads to vision loss and blindness in millions of people across the globe. It spreads easily through contact with eye discharge from infected people on hands and clothing, and through flies. If left untreated, chronic infections turn the eyelid inwards, causing intense pain and scarring of the cornea, which can lead to irreversible blindness.
Trachoma is preventable, and clean water is key to curbing the spread. When communities have access to clean water, people can clean their hands, faces and clothing more often, which prevents it from spreading.
In countries like Zambia, we work with Water Affairs (the government department responsible for water) to drill, rehabilitate and repair boreholes near where people live, work and go to school, so that whole villages have access to clean water. We also provide training to local volunteers in these communities in WASH (Water, Sanitation and Hygiene) and borehole repair and maintenance to ensure the clean water continues to flow. In areas where trachoma is endemic, we also work with partners to distribute antibiotics, which both treats and prevents trachoma.

It's another way that we work to address one of the root causes of avoidable vision loss, but it also helps us tie into improved health outcomes overall. Accessible clean water helps prevent dozens of infectious diseases. It also improves quality of life for women and girls, who are often tasked with the job of fetching water, which can take up hours out of the day and prevent them from participating in school, work or other activities. Moreover, clean water means people can grow vegetable gardens, raise livestock and keep entire families, and communities, happier and healthier.
When we invest in sight, we invest in education, productivity and dignity. To eliminate avoidable vision loss, vision care needs to be recognized as a public health priority and integrated into national health strategies. Operation Eyesight’s global experience – from rehabilitating boreholes in Zambia to collaborating with partners on new policies in Canada – demonstrates that integrating eye health into primary care, addressing environmental determinants like access to clean water, and empowering community health workers leads to sustainable, measurable outcomes. Policymakers have a critical role to play in building resilient health systems that ensure equitable access to vision care for all.
Read more about our approach to Hospital-Based Community Eye Health.
In the District of Netracona, the local vision centre is a lifeline for the community.
Located in the northern part of Bangladesh, many in the area experience poverty and lack access to basic necessities. Opened in 2021, the vision centre is a critical link that connects residents with eye health screening, prescription eyeglasses, specialist referral and other health services.
A bird’s eye view of the town’s skyline reveals one more thing that sets this vision centre apart: it’s covered in solar panels.
Powering a vision centre through a solar array is a forward-thinking solution in a country that stands at the forefront of climate change. Each year, Bangladesh faces rising sea levels and erratic weather patterns. Frequent floods, cyclones and droughts threaten not only the livelihoods of millions but also people’s health and well-being.
“In many ways, Bangladesh symbolizes the urgent need for global climate action,” explains Kashinath Bhoosnurmath, President & CEO of Operation Eyesight. “Changes in the environment have an impact on eye conditions and also present new challenges to healthcare systems. We need to take note and adjust the way we deliver care.”
Together with communities, we are setting a new standard in how healthcare systems can operate sustainably, improve lives and protect the planet.
Our eyes are incredibly delicate and sensitive organs, and emerging research confirms that eye health is susceptible to the environmental impacts of climate change. This is echoed by our healthcare staff and volunteers, working on the ground and in the community, who frequently witness firsthand the effects of climate change on public health. Extreme weather events such as wildfires, floods and dust storms disrupt access to essential eye care services and can cause direct eye injuries. Climate-related issues such as air pollution and drought can also increase the risk of various eye conditions.
Air pollution, for instance, is associated with a rising incidence of conjunctivitis and allergic eye reactions. And worsening wildfire seasons mean that heavy smoke more frequently blows into towns and cities, leading to complaints of burning, gritty and irritated eyes. What’s worse is that experts say the long-term effects of smoke on our vision are unclear. Studies out of China and India show that persistent exposure to high levels of pollutants made up of fine particulate matter, called PM2.5, is linked to an increased risk for age-related eye diseases like glaucoma and macular degeneration. While those studies focused on industrial pollutants, fine particular matter (PM2.5) is also a component of wildfire smoke.
In addition, the increase in ultraviolet (UV) radiation due to ozone depletion is linked to a higher risk of cataracts and other vision-threatening conditions.
The World Health Organization has identified climate-driven diseases, such as malaria and dengue fever, as potential contributors to visual impairment. Over the long term, droughts caused by climate change often result in food shortages, which are linked to vision loss.
In sub-Saharan Africa, where trachoma is a leading cause of blindness, climate change could worsen both the prevalence and severity of this disease. Since trachoma disproportionately affects women and girls, the climate crisis has broader implications – not only for eye health but also for development issues like gender equality.
The United Nations Sustainable Development Goals (SDGs) provide a blueprint for a more peaceful, prosperous and sustainable future, recognizing that Climate Action (SDG 13) is inextricably linked with other goals, such as those prioritized by Operation Eyesight: education, access to fresh water, gender equality, and good health and well-being.
“Climate change is both an environmental issue and a human health issue that is being felt across the eye health sector,” Kashinath says. “As the climate crisis intensifies, healthcare systems, especially those in low- and middle-income countries, must adapt to meet new challenges.”

A green approach to eye health care
Solar panels are just one example of how eye health services in the community can take steps to reduce greenhouse gas emissions, reduce carbon footprints and mitigate the effects of climate change.
In Elgeyo-Marakwet County, Kenya, our teams at Iten Eye Unit planted seedlings to help celebrate the first-ever National Tree Planting Day in November, 2023. Located in the arid western part of Kenya, where deforestation, overgrazing, soil erosion and water shortages have led to widespread desertification, it’s a step in the right direction.
In India, which is another of our countries of work, similar steps have also been recommended.
Bringing access to clean, fresh water to communities in sub-Saharan Africa has been one of our key strategies to improve health and reduce the transmission of blinding trachoma. In addition to educating communities about the importance of washing their hands, faces and clothes to reduce the transmission of disease, ensuring communities have access to sustainable, local water sources brings many other benefits as well.

For example, in Zambia’s arid Sinazongwe district, families who once faced food shortages due to drought are now able to grow backyard gardens, thanks to our work rehabilitating and drilling water boreholes.
By bringing access to fresh water and educating communities about the importance of water conservation, sanitation and hygiene, we’re improving health outcomes and empowering communities to reverse the effects of desertification in communities across sub-Saharan Africa.
“Sustainability goes hand-in-hand with empowering communities,” explains Kris Kelm, our Global Director of International Programs. “By educating communities on hygiene practices and supporting freshwater initiatives, we are enhancing the resilience of not just communities, but entire healthcare systems, in the face of climate change.”
Operation Eyesight is facing global challenges when it comes to climate change, but the solutions are driven by local communities.
“The climate crisis is having a very real impact on public health, and eye health is no exception,” Kris says. “Today, our work is focused on safeguarding eye health while minimizing the impact of our operations globally, and there is more work to be done.”
Public health and other development priorities will continue to be shaped by a range of issues, from food security to a shortage of healthcare personnel, to climate change issues.
“In coming years, the global eye health community’s response to climate change requires a thoughtful and coordinated approach from international organizations, as well as government agencies and policy makers,” explains Kashinath.
Kashinath says that more opportunities exist that will help address the eye health needs of underserved communities and drive environmental sustainability of operations, including:
“This way, our work is not only improving access to quality eye health services but also contributing to a healthier planet,” adds Kashinath.
Operation Eyesight’s partnership with communities to integrate environmental sustainability is more than a response to climate change; it’s a vision for the future of eye health.
Read our five-year Global Strategy to find out how we plan to continue meeting the eye health needs of communities in the face of climate change. Donate today to help us bring sustainable eye health solutions to communities that need it most.
As a community health volunteer, 28-year-old Faizunnahar spends her days bringing primary eye health care to the doorsteps of families who live in her area. She enjoys her job, but she knows that not everyone in her community approves of her work. In rural Bangladesh, where Faizunnahar lives, job opportunities for women are often limited by societal norms, and those who step outside of traditional roles often face criticism.
Nevertheless, with her family’s support, the young volunteer persists. She loves making an impact in her community, and she is proud to contribute to the family finances through the monthly stipend she earns. She is determined to build a better life for herself, her family and their young son.
Working with our partner organization, Symbiosis International, Faizunnahar goes door to door in nearby communities doing preliminary eye screenings and referring those with vision problems to the nearby Madarganj Vision Centre.

As a child, Faizunnahar remembers her father struggling with an eye problem. To get it treated, he had to travel from their village of Ruknai to the capital city Dhaka, nearly 200 kilometres away. His difficulties in getting treatment for his vision problems stayed with her and would later inspire her to seek out work in the healthcare sector.
When she first heard about the opportunity to become a community health volunteer, Faizunnahar worked quickly to reach out to a contact and put together a resume. After writing an exam, she was excited to learn she got the job. Since then, she has worked in maternal, newborn and child health, as well as primary eye care, for which we provided the training. She is proud of her achievements and says her greatest joy comes from knowing that her work is helping transform lives.
This International Women’s Day, we celebrate the thousands of women like Faizunnahar who are breaking barriers to help us deliver essential eye health care at the community level. As community health workers/volunteers, they have an opportunity to become leaders in their communities and act as catalysts for positive health outcomes. This employment improves their ability to become active participants in their family’s socioeconomic stability.
You can help support our mission to achieve gender equality in eye health care by sharing this post with friends and family, by learning more about the issues or by making a donation.
Anastasia, a 41-year-old mother of two teenage daughters, lives in Jei Krodua, in the Awutu Senya District of Ghana, where she earns a living brewing and selling asaana, a traditional local beverage. For nearly six years, she struggled with deteriorating vision, frequently endured pain and suffered from extreme sensitivity to light. These challenges made selling her drinks increasingly difficult and often, unable to see properly, accidentally gave customers too much change, realizing later that most did not return the extra money. “It wasn’t until I would go back home and calculate my sales that I would notice I had been cheated by some of my customers,” she recalled. One time, her impaired vision caused her to spill an entire batch of asaana while trying to place it on a table.

When Anastasia first began experiencing vision problems, she went to a nearby hospital, where she was diagnosed with pterygium — a growth on the eye’s conjunctiva. But, the pterygium was still immature, and she was advised to wait. By the time it had matured enough to be removed, her husband had grown older, fallen ill and was no longer able to work, leaving them without the means to pay for the surgery. “As a sole breadwinner and a mother of two teenagers who is also taking care of my husband, my meagre income could hardly take care of our daily needs, so undergoing a surgery was an impossible dream,” Anastasia shared.
Hope returned when Anastasia heard about an eye screening camp organized by Operation Eyesight. She attended, expecting little more than medication, but instead, she was diagnosed with a mature pterygium that could be removed through surgery at Operation Eyesight’s partner hospital Watborg Eye Services — free of charge, thanks to the generosity of donors. Anastasia underwent successful surgery, and she was also diagnosed with a refractive error and received prescription glasses at no cost.
With her vision fully restored and her business back on track, Anastasia could finally see a brighter future for her family.
“Though I feel that a mere thank you is not enough to express my appreciation, there is no other way to express to my joy except with a thank you. I am immensely grateful to Operation Eyesight for coming through for me.” – Anastasia
Your support can help restore vision and hope for someone like Anastasia. By giving the Gift of Sight, you not only honour your loved ones, but also extend the spirit of compassion and generosity to someone across the world.
Written with files from Dora Ewusi.
For millions of children worldwide, vision loss and blindness create barriers for learning, growth and opportunities — that's why child eye health is a focus this World Sight Day.
For 17-year-old Jennifer from Ghana, blurred vision made it difficult to keep up in class — until a simple pair of eyeglasses changed her life.
“I first noticed that I could not see objects clearly at a distance,” recalls Jennifer, who attends school in the Mfantseman District of Ghana’s Central Region. For three years, she struggled in silence, telling no one about her condition. As her vision worsened, she began relying on classmates to help her read the blackboard.
Relief came when Operation Eyesight hosted an eye health screening at her school. Diagnosed with a serious refractive error, Jennifer received a pair of prescription eyeglasses, free of charge.
Today, Jennifer is thriving and optimistic about her future. “I am happy with these new spectacles!” she says.
Jennifer’s story is far too common. Globally, nearly 450 million children and adolescents face similar vision challenges that could easily be solved with a pair of prescription eyeglasses. Additionally, 40 per cent of children who are blind could have had their eye conditions prevented with access to eye health care, according to the International Agency for the Prevention of Blindness (IAPB).
Shining a light on child eye health on World Sight Day
On October 10, the global eye health community will celebrate #WorldSightDay, encouraging everyone to prioritize their eye health. This year’s theme highlights the importance of eye care for children, inspiring young people to 'love their eyes'.
“Every day, preventable and treatable eye health issues cause children to miss out on learning and social opportunities,” says Kashinath Bhoosnurmath, President and CEO of Operation Eyesight. “They do not just deserve but have the right to a happy childhood. Healthy eyes enable kids to learn, play, and thrive, setting them on a path for life.”
Untreated vision loss can have lifelong consequences, especially for children in low- and middle- income countries, who are five times less likely to attend school if they have a vision impairment, states the IAPB. Providing accessible and quality eye care helps meet the United Nations (UN) Sustainable Development Goals (SDGs) of Quality Education (SDG 4) and Good Health & Well-being (SDG 3).

School Eye Health Programs: Reaching children where they are and raising awareness of programs on World Sight Day
In 2023, Operation Eyesight screened more than 240,000 students at 1,133 schools across South Asia and sub-Saharan Africa. By training teachers and healthcare workers to identify vision problems, we ensure youths like Jennifer receive the care they need.
Child eye health is about more than providing eyeglasses; it’s about creating long-term solutions. In places like Ethiopia, Kenya and Zambia, trachoma is a leading cause of vision loss. If left untreated, this bacterial infection can lead to irreversible blindness. Along with mass drug administrations (MDAs) to clear infections, our teams also bring communities local access to fresh water and educate people about the importance of washing their hands, faces and clothing to reduce transmission of the infection.

Yashwant Sinha, our Director of International Programmes, says Operation Eyesight’s clean water projects have had a ripple effect in the lives of female students.
“In many communities across sub-Saharan Africa, the task of hauling water falls to women and girls. Local access to fresh water has boosted school attendance, because girls no longer have to spend hours fetching water,” Yashwant says. “In many communities, attendance of girls at school has improved.”
He adds that in Ethiopia, these benefits have been bolstered by Water, Sanitation and Hygiene (WASH) programs both in the community and at schools, as well as menstrual hygiene training, including how to create reusable sanitary pads using local materials.
These efforts also support the UN SDGs related to Clean Water and Sanitation (SDG 6) and Gender Equality (SDG 5).
A comprehensive approach to eye health
Our work extends beyond schools. Operation Eyesight’s global team of Community Health Workers (CHWs) enables us to be present in the community and reach patients who otherwise would not have access to quality eye health care.
By conducting door-to-door screenings, CHWs help families understand the importance of seeking eye care, ensuring that no man, woman or child goes without eye health screening and referral if needed. Through public health education, we also promote awareness about hygiene and overall health, linking residents with local healthcare resources.
“Healthy eyes are just one part of a person’s overall health and well-being, and we are also focused on addressing other determinants of eye health,” Yashwant explains.
“Our CHWs and other local staff connect new moms with pre- and post-natal care and also connect families with immunization clinics to help give kids the best start.”

Addressing complex conditions early
Some vision issues, like Retinopathy of Prematurity (ROP), need intervention much earlier. ROP is one of the leading causes of vision loss in children in India, and preterm infants are at high risk of developing this condition which leads to lifelong blindness.
Shabana, from a small village in Uttar Pradesh, India, delivered her son Aarsh when she was only seven months pregnant. Thanks to Operation Eyesight’s partnership with C.L. Gupta Eye Institute (CLGEI) in nearby Moradabad city, Aarsh was screened and treated for ROP, saving him from a life without sight.
“Aarsh’s journey is a testament to the transformative power of our ROP screening program,” says Lokesh Chauhan, Deputy General Manager at CLGEI. “Aarsh’s bright eyes now reflect a world of possibilities.”
Ocular cancers such as retinoblastoma not only cause blindness but can also be fatal. In India, retinoblastoma accounts for about three per cent of all cancers affecting children under five, and it is reported in an article in the Indian Journal of Ophthalmology that there are about 1,500 new cases reported each year.

Timely treatment of this cancer can save the lives of more than nine out of 10 children suffering from this disease, including children like Alok, pictured above. In many cases, a child’s vision can also be saved, but early screening and treatment are essential. Thanks to the help of our generous donors, in 2015, Operation Eyesight, in partnership with LVPEI, opened one of the few facilities in the world that specializes in treating ophthalmic tumours in both children and adults.
Tapobrat Bhuyan, our Programme Manager in India, adds that untreated vision loss can also have long-term effects on children’s self-esteem.
“Clear vision and healthy eyes open the door of possibility. For a child, it’s a chance to have a full childhood, which has long-term impacts for their trajectory in life,” Tapobrat explains. “Vision loss and blindness have been proven to prevent social inclusion and can negatively impact mental health.”

Looking ahead: World Sight Day 2024
Vision is crucial for a child’s development — whether in the classroom, playground, or at home. It’s no surprise that 80 per cent of a child’s learning is visual, according to multiple studies. Wherever they live, access to quality eye health care helps give young people the best possible start in life, paving the way for success for years to come.
Access to eye health care isn’t just an issue in low- and middle-income countries. Globally, myopia is on the rise. Commonly known as nearsightedness, myopia makes it difficult to see distant objects clearly. The number of children experiencing myopia is increasing, driven by excessive screen time. In 2020, 60 per cent of children in Asia and 50 per cent in Europe had myopia.
Reducing screen time and scheduling regular eye exams are simple steps we can take to protect our children’s vision. A 2021 study found that extended screen time is associated with a 30 per cent higher risk of myopia, which requires prescription eyeglasses. When combined with excessive computer use, the risk more than doubles, reaching approximately 80 per cent.
In Canada, some provinces offer free eye exams to children and seniors as part of provincial health care. Access to eyeglasses is one of the most effective health interventions for kids.
Download our child eye health resources on our World Sight Day page to learn more and help the children in your life love their eyes.
World Sight Day 2024 is a chance to focus on our kids’ eye health and help children and adolescents everywhere love their eyes.
Help all children love their eyes this World Sight Day
You can also help ensure that no child is left behind due to preventable vision loss. Together, we can create a world where every child has access to quality and affordable eye health care. Make a donation today to help bring sustainable eye health solutions to children living in communities that need them most.
Between textbooks, whiteboards and videos in class, most of the information that’s presented to kids at school is visual. So what does that mean for a child who can’t see clearly?
In countries where eye health care is difficult to access, a simple eye condition like myopia (nearsightedness) can cause a student to fall behind and even drop out of school, which in turn could affect the child’s income for the rest of his or her life.
Ensuring that Quality Education is available to all children is one of the 17 Sustainable Development Goals set by the United Nations’ 2030 Agenda. We’re working towards this goal by ensuring that more children get the eye health care they need to thrive at school and take charge of their education.
According to a survey by the World Bank, children with visual impairments in sub-Saharan Africa are five percentage points less likely to ever be enrolled in school or to complete primary school. They are six percentage points less likely to be literate.1
The links between academic performance and visual impairment can be harder to draw given the complexity of the issue, but one survey from francophone countries in Africa found that primary school students – who self-reported difficulties with their vision – performed worse on standardized tests in math and reading in all but one of the 10 participating countries.2 Similarly, a Stanford study of 20,000 fourth and fifth graders in rural China found that eyeglasses boosted the standardized test scores by 18 per cent over six months.3

Even studies from higher income countries, where children have better access to eye health care, show that students with poor vision tend to read more slowly than their peers and are more likely to report that they don’t like reading.4 Visual fatigue is a likely culprit for both, and the resulting headaches and tiredness that these kids experience are also thought to play a role in behavioral issues at school.
Roughly 22.16 million children ages 14 and under have Moderate to Severe Vision Impairment (MSVI) and 44.6 million have mild vision impairment, according to a panel of global health professionals called the Vision Loss Expert Group.5
Only 20-50 per cent of the children who need prescription eyeglasses worldwide actually own a pair.6 Often, this is due to a lack of access to eye health care. In rural, remote or underserved communities, especially in low- and middle-income countries, many kids don’t get regular eye exams or have access to prescription eyeglasses and other treatment. This could be due to financial constraints, lack of education about the importance of eye health, or simply because there aren’t any optometry clinics nearby.
Across lower-income communities, schools may also lack electricity or lighting, making it even more difficult for a student with vision impairment to read information written on a blackboard. Lack of adequate lighting at home can also cause difficulties in completing homework. For a secondary student who is already falling behind in class, not being able to finish homework in a timely manner could end their school career, and cause them to drop out early.

Isaac Baffoe, who manages our school eye health programs in Ghana, says one student’s story really stuck with him. The girl reported that her eyesight started to fade when she was about 12 years old, and by age 15 she had severe vision impairment. For years, she relied on a classmate to read the blackboard out loud to her during class. Isaac often wonders what would have happened to her if her friend hadn’t been so helpful, or even more importantly, if our school eye health program hadn’t reached her school and she hadn’t gotten prescription eyeglasses.
Our field staff hear a lot about the difficulties that students face before they get eyeglasses. One student in Ethiopia reported that she and her friend were frequently scolded when the friend read the blackboard notes aloud to her. Others reported that their grades dropped sharply, or that they lost interest in their studies. Many children say that they asked their parents to take them to the eye doctor, but due to tight finances or difficulty in reaching a clinic, they weren’t able to get the eye care they needed.
The good news is that, with your ongoing support, we are changing all of this – one school and one child at a time.

Part of our goal at Operation Eyesight is to reach every single member of a community with eye health care, ensuring that nobody gets left behind. Increasingly, we’re screening school-aged children for eye issues right in the classroom.
In 2023 alone, our school eye health programs helped us screen more than 240,000 students in Bangladesh, Ethiopia, Ghana, India, Kenya, Nepal and Zambia.
In Kenya, we’ve partnered with the United States Agency for International Development’s (USAID’s) Child Blindness Program and Peek Vision to deliver an innovative program where teachers are trained to do the initial eye health screenings using a simple smartphone app. This allows us to screen more students overall, while still providing referrals to those children identified with eye problems to get a complete eye exam with a healthcare professional.

In Ghana, we train community health nurses to help deliver our school eye health programs, also in partnership with USAID and with funding from the Church of Jesus Christ of Latter-day Saints and Latter-day Saints Charities. In addition to conducting school eye health screenings, the nurses provide the students with eye health education sessions, where they learn how to prevent eye injuries and infections and learn about various conditions, like refractive errors (the need for eyeglasses). By making sure children have basic eye health information and know where to go for subsidized eye care, whole families are made aware of the services that are available to them.
Isaac, who has been on hand during several of these school screening events, says the children are always very eager to get involved. “The children show lots of interest. They want to participate,” he explains. “During all the screenings we’ve attended to audit, the children are very cooperative, they really want to know what is going on.”
He adds that it’s not just the students who are happy with getting a pair of eyeglasses.
“It’s not only a relief to the children, but also to the teachers,” he says, “because it also made their work difficult to spend extra time with these children who were struggling with their studies prior to receiving eyeglasses.”
In November 2020, the borehole in the Zambian village of Kangwa broke down. The COVID-19 pandemic was in full swing, and the need for clean water was more urgent than ever. For Natasha, a teenager who was in high school at the time, the breakdown had devastating consequences. As the family member tasked with fetching water, Natasha now had to walk several kilometres each day to complete the chore, meaning she could no longer attend school. She wasn’t alone – other teenage girls in her community were in the same situation.

When our team in Zambia found out about the broken borehole, they sprang into action and quickly got it fixed. They were well equipped to do so, because we have been working with communities to repair and drill boreholes for many years to curb the spread of trachoma.
Trachoma is a bacterial eye infection that’s common in areas with water shortages and crowded living conditions. The bacteria spreads easily through contact with eye discharge from infected people on hands and clothing, and also through direct transmission by flies. If left untreated, it can cause severe pain, vision loss and even blindness. In fact, it is the leading infectious cause of blindness worldwide.
When we work with communities in areas of Zambia, Ethiopia and Kenya where trachoma is endemic, we ensure that water and sanitation issues are part of our intervention. In communities like Kangwa, this means training local volunteer teams to help maintain and repair broken boreholes, and training community WASH (Water, Sanitation and Hygiene) teams to educate their neighbours about preventing trachoma transmission in the home.

In order to ensure that girls have equal access to quality education, clean water and sanitation facilities must be part of the solution. (Watch this video to learn more about the ripple effects of clean water.)
Myopia (nearsightedness) rates are on the rise all over the world. In 2020, the global prevalence was 30 per cent. It’s estimated to rise to 50 per cent by 2050.7
In China, where the rise in myopia in children is being described as an epidemic, the government has rolled out a nation-wide strategy to curb the growth, which includes school-based eye screenings, public health education campaigns, a reduction in homework and an increase in time spent outdoors.8
As suggested by China’s strategies, many of the factors contributing to the rise of myopia are likely due to modern lifestyles: more time spent indoors, doing near-work like homework, and more time spent parked in front of digital devices.
But there may be more at play in the phenomenon, including environmental risks like increasing urbanization and changing diets. As low- to middle-income countries become more urbanized and educational pressures mount, children everywhere are at increased risk of developing the refractive error. In parts of Africa and Asia where families already face difficulties accessing eye health care, the gap between eye health services and those in need of treatment will continue to grow.
As part of our 2024-2028 Global Strategy, we are committed to providing eye health care and clean water to more children so that they can take full advantage of any educational opportunities they are presented with. This means integrating WASH projects with school eye health projects and rolling out more school eye health programs across our countries of work.
We have already seen much success with our school eye health programs in countries like Kenya and Ghana, where we’re working with the local ministries of health and education. Now, it’s time to scale our efforts to more schools, more districts and more countries. With your ongoing support, we can expand our reach and improve the quality of life for more kids around the world.
Donate today and help us restore sight and prevent blindness for more children. The Gift of Sight is the gift of education and the gift of opportunity. Thank you for your support!