

For most of her life, Napolo, from Narok West Sub-county near the Kenya-Tanzania border, lived with constant eye pain. Now 78 years old, she first noticed discomfort in her 30s. Her eyes often felt irritated, as if filled with sand, and she experienced tearing and discharge that made it difficult to see. This attracted flies, but Napolo had no access to clean water to wash her face.
Napolo wasn’t aware that she was suffering from trachoma, a bacterial infection of the eye and the leading cause of blindness in areas with shortages of water and crowded living conditions. The bacteria spreads easily through contact with eye discharge from infected people on hands and clothing, and also through direct transmission by flies.
If left untreated, trachoma causes the eyelids to turn inward, making the eyelashes rub painfully against the surface of the eye. This causes permanent scarring of the cornea and irreversible vision loss.
Without access to regular health care, Napolo turned to traditional remedies. Her family members would pluck out her eyelashes to help ease the pain, but the relief never lasted. The irritation always returned, and over time, Napolo’s vision became worse.
In her Maa community, many people had similar symptoms, and plucking one's eyelashes out was considered normal. Health workers occasionally visited their community, but Napolo often missed them because she was always out looking after her animals, sometimes even crossing over the border to let the animals graze in Tanzania. She somehow managed despite her diminishing vision and increasing pain.
One fateful day, an Operation Eyesight-trained Community Health Promoter visited Napolo’s home – and the visit changed everything.
You see, for many years Operation Eyesight has been working to eliminate trachoma in communities like Napolo’s. Through the Kenya Trachoma Elimination Program, funded by Sightsavers International, Operation Eyesight and partners are working to eliminate trachoma in Narok West Sub-county and the entire country by 2028. With this support, and in collaboration with the Narok County Department of Health, we launched a door-to-door screening initiative to identify remaining cases of trachoma trichiasis – the painful late stage of the disease. We provided training and resources for local Community Health Promoters. They screen people in their communities and refer those in need of eye care to our nearest partner facility.
During a community screening in November 2024, Napolo was identified and referred to Talek Health Centre, an outreach site that provides surgical treatment for trachoma patients. At the health centre, the ophthalmic team examined Napolo’s eyes and confirmed her diagnosis.
Napolo agreed to undergo eyelid surgery to correct her inward-turned eyelids. The procedure was successful, and her recovery brought immense relief, preventing further damage to her eyes and preserving her remaining vision.
“I have longed for this comfort for decades. There is no more discomfort, and I can open my eyes freely,” Napolo said. “I thank Operation Eyesight and the doctors who assisted me, and I will definitely refer anyone in my community that has the same problem so that they can be assisted.”
Napolo’s story shows how access to quality eye care can transform lives.
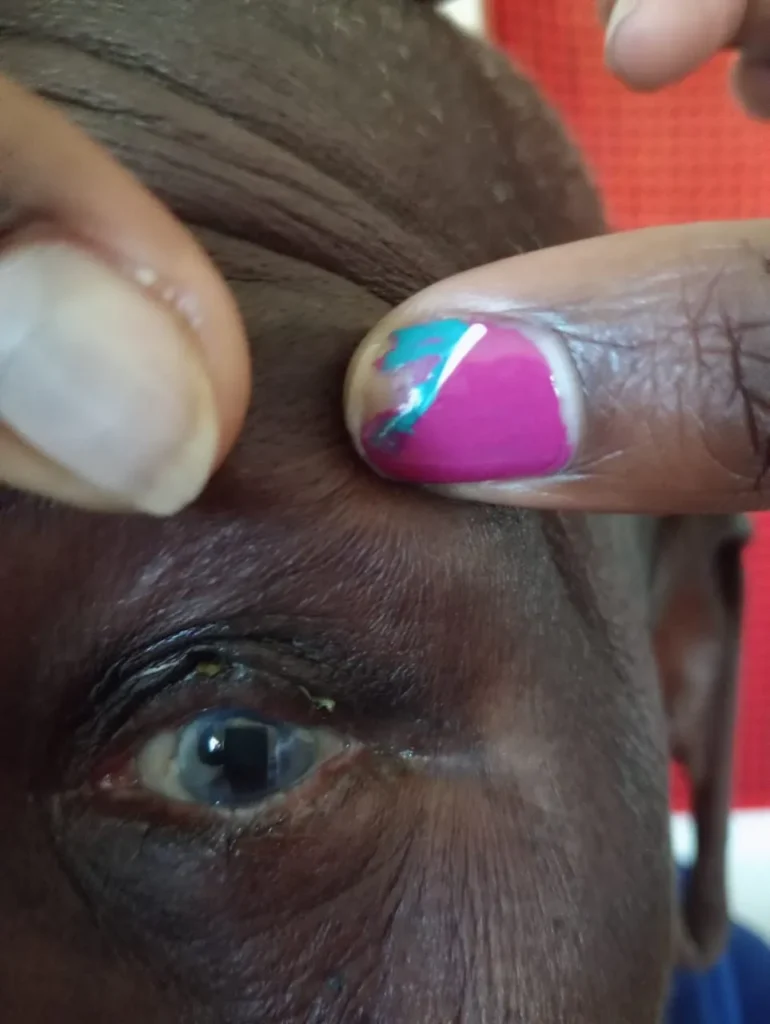
Did you know? Trachoma is the leading cause of infectious blindness.
Currently, 103 million people live in trachoma endemic areas and are at risk of trachoma blindness, and presently 1.9 million people are experiencing vision impairment or blindness due to the disease.1 It is found in 32 countries, in areas with shortages of clean water and crowded living conditions. Caused by the bacteria Chlamydia trachomatis, trachoma is spread by eye-seeking flies and personal contact. Children and women are at particular risk.
Operation Eyesight follows the World Health Organization-endorsed SAFE strategy, which has proven effective in eliminating trachoma. The SAFE strategy is a comprehensive treatment and prevention program that includes Surgery to treat the late stage of the disease, Antibiotics to eliminate infection, Face washing and hygiene education, and Environmental change including wells and latrines.
Join us in supporting programs that bring vital vision care to people like Napolo and also address the root causes of vision loss. Together, we can eliminate trachoma and ensure everyone has access to the eye care they deserve. Give the Gift of Sight today. Join us in supporting programs that bring vital vision care to people like Napolo and also address the root causes of vision loss. Together, we can eliminate trachoma and ensure everyone has access to the eye care they deserve. Give the Gift of Sight today.
If you sprain an ankle or come down with a bad cough, your first stop is usually your family doctor. But when it comes to blurry vision, the path to care often looks very different. Around the world, eye health is still treated separately from primary health care, creating gaps that leave people without the vision help they need. Even in countries with universal health coverage, you might receive a complex eye surgery at no cost, yet pay out of pocket – or use private health insurance – for something as simple as a pair of eyeglasses.
At Operation Eyesight, we believe this needs to change. That’s why we’re working to strengthen areas of overlap between primary eye care and primary health care in our countries of operation. That means supporting the World Health Assembly’s integrated people-centred eye care (IPEC) resolution by working to integrate eye health into national health systems – and increasing access to free or subsidized eye health care.
It also means addressing the root causes of avoidable vision loss. In some regions in Africa, we bring fresh water and hygiene education to communities to help prevent infectious eye conditions. We also work to make sure our services offer more than just eye care, but can also link patients to other types of health care.
Health conditions rarely exist in silos – and vision loss is no exception. Diabetes, for example, increases the risk of eye conditions like cataracts. For 15-year-old Vanessa in Zambia, blurry vision was one of the first signs of the disease. When she started having problems reading the blackboard at school, a teacher sent her to our vision centre in her community of Matero for a checkup. From there, she received a referral to our partner hospital, where she learned that she not only had cataracts, but diabetes as well. Doctors helped her get her blood sugar levels under control, and then she got cataract surgery. Today, she is managing her diabetes and thriving in school, with dreams of becoming a doctor.

Vision problems can also cause a downward mental health spiral. Benson, a farmer in Kenya, lost his ability to work due to poor vision. As a result, he became angry and depressed, then turned to alcohol and drugs to cope with his situation. Luckily, his family got him into a drug and alcohol rehabilitation facility, where a visiting doctor diagnosed him with cataracts. Benson underwent surgery on both eyes, provided free of charge thanks to the support of our donors, and can see clearly now. Buoyed by his miraculous recovery, Benson finished up his time at the rehabilitation facility and happily threw himself back into farming.
In Canada, where Operation Eyesight is based, navigating eye care can be confusing. While the Canada Health Act covers medically-necessary eye health services, routine vision care like eye exams and prescription glasses often isn’t part of the deal. That leaves provinces and territories to fill in the gaps, and the result is a patchwork system. For example, seniors in Ontario get routine eye exams covered once they hit 65, but in Newfoundland and Labrador, those same seniors might have to pay out-of-pocket. It’s inconsistent, and it’s especially tough on vulnerable populations.
There is some support through the Federal Non-Insured Health Benefits (NIHB) program, which covers eye exams and eyewear for eligible First Nations and Inuit individuals. But even that has its hurdles: remote communities, limited healthcare infrastructure and cultural differences that make accessing care more complicated than it should be.

The passage of the National Strategy for Eye Care Act in 2024 was a major step forward in addressing these issues. As chair of the Canadian Eye Health Coalition, Operation Eyesight is helping shape a national framework that prioritizes equitable access to vision care. Our Global Director of International Programs, Kris Kelm, explains why it’s important that we have a seat at the table during the consultation period and beyond.
“We know that there will be many voices in this conversation with diverse interests, and we want to ensure there is representation from patients who have the least means and the least ability to access vision care,” he says. “The fact that we have over 60 years of experience working in this sector gives us a strong background to speak credibly to how we need to approach things in Canada, and our community partners can provide valuable insights to help shape eye care for all.”
He adds that Canada can learn from some of our countries of work, where eye health has been better integrated into the overall health systems and other public frameworks. As an example, he points to Ghana, where we work with the ministries of health and education to screen and treat students for eye conditions in the public school system. We have similar programs in Kenya and Zambia, too.
Another example is in India, where we are working with state governments to establish vision services in pre-existing government health centres. Building the capacity of vision care facilities within the country’s national health care system ensures that services reach the most underserved populations, as patients who are able to pay most typically seek care at for-profit facilities, rather than attending government services.
Shakuntala, in Madhya Pradesh, India, spends her days walking door to door through villages in her region, checking in on the health and well-being of families. She’s one of the million-strong network of Accredited Social Health Activists (ASHAs), employed by the Indian government, who deliver primary health care at the community level.

Her work includes providing pregnancy advice, supporting newborn care, educating parents about vaccinations and vitamins for children, and making all kinds of referrals to local clinics and hospitals. In 2022, Shakuntala added another set of skills to her toolkit: conducting primary eye health screenings, thanks to training provided by our Operation Eyesight team, in partnership with the Government of Madhya Pradesh. Shakuntala learned to measure visual acuity using an eye chart. She also learned to identify the signs and symptoms of various eye conditions. Once she identifies a patient with a possible eye condition, she refers them to the base hospital for diagnosis and treatment. In the meantime, she continues to provide advice and referrals on nutrition, vaccinations, prenatal care and other health concerns.
Shakuntala is just one of the thousands of community health workers we work with across the globe. In all our countries of work, we partner with existing health systems to recruit community health workers, mostly women, to help us deliver our programs. The health workers develop strong ties within the communities, resulting in high acceptance and trust in our programming.

Mabel, a community health nurse in Ghana, was trained in primary eye care so that she could identify eye health issues in addition to her regular duties. She says that being able to screen people at their home allows her to reach many women and girls who probably wouldn’t have left the village to seek eye health care, due to household responsibilities.
Anyone who has had a case of pink eye knows that having red, inflamed and itchy eyes isn’t much fun. But in some parts of the world, an eye infection can be a much more serious problem. Trachoma is an infectious eye disease that leads to vision loss and blindness in millions of people across the globe. It spreads easily through contact with eye discharge from infected people on hands and clothing, and through flies. If left untreated, chronic infections turn the eyelid inwards, causing intense pain and scarring of the cornea, which can lead to irreversible blindness.
Trachoma is preventable, and clean water is key to curbing the spread. When communities have access to clean water, people can clean their hands, faces and clothing more often, which prevents it from spreading.
In countries like Zambia, we work with Water Affairs (the government department responsible for water) to drill, rehabilitate and repair boreholes near where people live, work and go to school, so that whole villages have access to clean water. We also provide training to local volunteers in these communities in WASH (Water, Sanitation and Hygiene) and borehole repair and maintenance to ensure the clean water continues to flow. In areas where trachoma is endemic, we also work with partners to distribute antibiotics, which both treats and prevents trachoma.

It's another way that we work to address one of the root causes of avoidable vision loss, but it also helps us tie into improved health outcomes overall. Accessible clean water helps prevent dozens of infectious diseases. It also improves quality of life for women and girls, who are often tasked with the job of fetching water, which can take up hours out of the day and prevent them from participating in school, work or other activities. Moreover, clean water means people can grow vegetable gardens, raise livestock and keep entire families, and communities, happier and healthier.
When we invest in sight, we invest in education, productivity and dignity. To eliminate avoidable vision loss, vision care needs to be recognized as a public health priority and integrated into national health strategies. Operation Eyesight’s global experience – from rehabilitating boreholes in Zambia to collaborating with partners on new policies in Canada – demonstrates that integrating eye health into primary care, addressing environmental determinants like access to clean water, and empowering community health workers leads to sustainable, measurable outcomes. Policymakers have a critical role to play in building resilient health systems that ensure equitable access to vision care for all.
Read more about our approach to Hospital-Based Community Eye Health.
For most of his adult life, Abraham made a living as a cobbler, supporting his wife and raising six children on his earnings. But several years ago, he started having trouble threading needles. Initially, he pricked himself repeatedly, and eventually, he couldn’t get the needles threaded at all. Due to his poor eyesight, Abraham had to shut down his shoe repair business.
His story is a common one. Global estimates suggest that people with moderate to severe vision impairment are about 30 per cent less likely to be employed than those with good eyesight.1 For lack of a pair of eyeglasses, for want of a simple cataract surgery, millions of people are unable to work. It can keep entire families stuck in the cycle of poverty.

Abraham’s story has a happy ending. After meeting a community health volunteer during a door-to-door eye health screening, he was diagnosed with bilateral cataracts and got sight-restoring surgery on both of his eyes at one of our partner hospitals. He started taking in shoes for repair once again.
But many people won’t get back to work like Abraham did. And that’s because basic eye care isn’t available or accessible to them. According to estimates, about 2.2 billion people worldwide have vision impairment, and in roughly half of those cases, the vision loss could have been prevented or hasn't yet been treated.2
For many people across the globe, the neighbourhood optometry clinic simply doesn’t exist. While people in Western Europe enjoy a ratio of one optometrist to every 3,877 people, countries in central sub-Saharan Africa reported a ratio of one to every 1,198,141 people, according to a 2023 study.3 Even when there is an eye care provider in a nearby city, the barriers to reaching them can be insurmountable for some people living in remote and rural areas. Many can’t afford the bus or train fare, let alone the fees for diagnosis and treatment. And for women and children, travelling alone can be dangerous, so they often need to wait for someone – usually the family breadwinner – to take time off work to escort them. For those with seriously impaired vision or other disabilities, travel might be nearly impossible.
Every day, the community health workers who do eye screenings on our behalf meet people who have previously tried to solve their vision issues without success. Many patients had visited the nearest healthcare provider, often a local dispensary, and were sent home with eyedrops or told their vision couldn’t be treated. Some had bounced around from clinic to clinic, others had resigned themselves to living out their days in blindness. That is why we are working hard to provide eye health care services at the community level.
By connecting people with our partner vision centres and hospitals, helping cover fees and offering safe transportation to the hospital, we can help restore vision to people who may never have gotten treatment otherwise. It’s just one of the ways we are working towards the United Nations Sustainable Development Goal number one: No Poverty. By addressing some of the root causes of poverty, like poor eyesight, we can help people stay employed and stay in school.
The global productivity loss attributed to impaired vision is estimated at US $411 billion annually.4 And those effects can be seen on the individual level as well.
A recent study looking at workers with presbyopia between the ages of 35-65 in Bangladesh found that those who had reading glasses made 33 per cent more than those who did not.5 The study, published in PLOS ONE, tracked the incomes of more than 10,000 participants who work in near-vision intensive occupations – like tailors, mechanics and carpenters – over eight months. Half of the participants received reading glasses right away, while the control group only got a pair after the eight months of data collection. The eyeglasses themselves cost only about US$3-4 per pair but had the potential to transform the lives of the workers.
Another study of tea pickers with presbyopia in India found similar results in 2018.6 In that case, the three-month study found that a pair of reading glasses increased productivity for the plantation workers – who are paid by the kilogram of leaves picked – by about 22 per cent, and 32 per cent for those over the age of 50.
As these studies show, addressing vision loss can increase productivity and provide greater economic opportunities for individuals.
Like many other health issues, it can be difficult to untangle the relationship between low incomes and eye health problems. Poor vision can lead to poverty because people often lose or quit their jobs when they’re no longer capable of doing them effectively or safely.

Take Junmoni in India, for example. The mother of two dreamed of sending her daughter to college with her earnings making handwoven fabrics on her loom. But when her vision became blurry, she had to stop weaving. Money got so tight that she was on the brink of selling her handloom. Fortunately she met a community health worker who told her she just needed to visit the local vision centre to get a pair of eyeglasses. Junmoni now wears her prescription eyeglasses while working at her handloom, her dreams for her daughter back on track.
But just as vision loss can lead to poverty, the opposite may also be true.
An infectious eye disease, called trachoma, continues to cause vision loss and blindness in dozens of countries around the world. It is widespread in some rural areas, and also in regions where there are high rates of poverty. The bacteria spreads through personal contact, via hands, clothes and bedding, and by flies that have been in contact with discharge from an infected person. It is most common in areas where people don’t have access to clean water or have to travel long distances for water.
If left untreated, trachoma causes the eyelashes to turn inward and scratch the cornea, leading to severe pain, vision loss and even blindness.
The spread of trachoma can be managed when people have access to clean water, allowing for more frequent hand and face washing, and the cleaning of clothing and bedding. Antibiotics can also help prevent and treat trachoma in areas where it is endemic.

We work with partners and communities in Ethiopia, Kenya and Zambia to prevent the spread of trachoma by helping establish water boreholes and latrines and administering antibiotics.
Ninety per cent of vision loss is preventable or treatable, but people living in underserved communities are more likely to go blind. In fact, 90 per cent of people with vision loss live in low- and middle-income countries, which is why we’re working in these areas.
Lack of education is another factor that keeps vision loss in lockstep with poverty. Some people don’t seek eye health care simply because they believe their condition is untreatable. Many older patients believe that vision loss, even blindness, is just an inevitable part of aging. In some communities there may be additional fear or distrust of medical authorities based on previous experiences, myths or other cultural stigmas.
By reaching people in their homes and communities through door-to-door eye screenings and eye camps, we can offer basic eye health education and choice to those who might never get treatment otherwise. And in cases where a patient might be hesitant to get surgery, our community-based approach enables health workers to continue counselling patients over weeks and months, reassuring them, explaining the benefits of a procedure and often convincing them to get treatment in the end.
Another way we work to prevent the devastating effects of vision loss is by making sure the youngest people in our project areas learn about eye health. By offering eye screenings and education in schools, organizations like ours can reach thousands of families through their children, who go home brimming with excitement over the vision test they took at school, and what they learned about eye health. By providing children with referrals to the nearest vision centre or partner hospital, the whole family is made aware of the services that are available to them.

The effects of a cataract surgery often ripple down through the beneficiary’s entire family. We hear of many young women who have given up jobs or dropped out of school to care for a senior family member who has gone blind. Once the family member has had their vision restored through cataract surgery, they often regain their independence, freeing up their caregiver to devote that time to work, school or other economic opportunities.
And parents who have had their vision problems corrected, like Junmoni, are better placed to keep their children in school longer, and even send them off to advanced education, potentially lifting future generations out of poverty.
Finally, children with vision problems who get corrective eyeglasses or treatment fare better at school. In fact, prescription eyeglasses have been shown to have a greater impact on academic achievement than other health interventions, like nutrition and deworming programs.7 This is why we are currently expanding our school eye health programs, so we can help more children thrive in school so they can get the best possible start on their working lives.
While many organizations like ours are collaborating with partners, governments and funders to address vision loss and blindness, aging populations and population growth mean that the problem will increase if we don’t act quickly. Some estimates say that by 2050, half of the global population will have myopia.8
You can help us continue our mission to prevent blindness and restore sight by following us on our social media accounts, signing up for our newsletter and sharing what you’ve learned with friends and family. Join our global community today.
At first, a trachoma infection looks a bit like a case of pink eye: red, irritated eyes, maybe some swelling and discharge1. But for many people in the world, a trachoma infection is a serious concern. If left untreated, it can lead to severe pain, vision loss and even blindness. The bacteria that cause trachoma spread through direct personal contact, through shared towels and clothing, and through flies that have been in contact with an infected person. And there’s a simple solution for reducing its spread…
Clean water.
When communities have access to abundant clean water, they can wash their hands and faces regularly, do laundry more often, and prevent the otherwise relentless transmission of the disease. That’s why we are working hard with communities and partner organizations to make sure that the people in our project areas have access to a local, sustainable clean water source.

There’s been a lot of good news in the eradication of trachoma in recent years. In 2023 alone, Benin, Iraq and Mali each received certification from the World Health Organization (WHO) for eliminating trachoma as a public health problem. Also, the number of people at risk of getting the infection fell from 125 million in 2022 to 115.7 million in 2023, a significant reduction.2
But the hard work must go on.

Ethiopia has some of the highest rates of trachoma worldwide, with the prevalence in the Amhara Region estimated to be nearly 63 per cent. In that country, trachoma is the second leading cause of blindness overall.3
Trachoma continues to infect people in 42 countries and has caused blindness or visual impairment in roughly 1.9 million people. It remains the leading infectious cause of blindness worldwide. And the effect on the workforce in these countries is huge. According to a recent paper by the WHO, the loss of productivity due to trachoma costs somewhere between US $3-8 billion each year.4
To people like Stephen, in Narok County, Kenya, having trachoma meant not being able to support his family. The father of four, who works as a motorcycle courier, struggled with the infection for years. He tried eye drops, eyeglasses and several surgeries before the trichiasis in his right eye, caused by repeat trachoma infections, was fully resolved.
Since undergoing a successful final surgery at one of our partner hospitals, the young man now acts as an eye health ambassador in his community, making sure people know what the infection is, the role of hygiene in stopping its spread, and how to get it treated.
Years of repeat infection from trachoma causes scarring to the eyelid. This scarring can be so severe that the eyelid turns inward, causing the eyelashes to rub against the eyeball. This leads to severe pain, light intolerance and scarring of the cornea.
If left untreated, the damage to the cornea can cause vision impairment, usually between the ages of 30 to 40 years5, although it can happen in children as well. Trachoma causes 1.4 per cent of blindness globally.6
Women become blind from trachoma four times as often as men. This is likely due to frequent infections they get while caring for small children, who often pass trachoma on to others.
At Operation Eyesight, we follow the WHO’s SAFE strategy for controlling and preventing trachoma. SAFE stands for:
S: Surgery to treat trichiasis (the painful late stage of the disease)
A: Antibiotics to eliminate infection
F: Face washing and hygiene education
E: Environmental improvement including wells and latrines

The foundation for the strategy is environmental improvement, namely – providing access to clean water. Over the decades, we’ve worked with communities to rehabilitate and drill hundreds of boreholes. In recent years, most of our work with water has been concentrated in Zambia and Kenya, but we are also getting involved in more water projects in Ethiopia as we expand our programs there.
Along with drilling and rehabilitation, we work with local governments to make sure people can fix the boreholes when they break down. In Zambia, that means financing the training of volunteers called Area Pump Minders (APMs) to do routine maintenance and repair of boreholes. The program helps ensure that there is a system for repair work, with locally-available toolkits and spare parts, and that monitoring of the water supply is happening at the village level. In addition to helping their communities, some of the APMs go on to find paid work repairing privately-owned boreholes. Over the last two years, we’ve seen several women join the traditionally all-male teams, and we hope to recruit more in future.

The community involvement doesn’t stop there. We also work with volunteers to form WASH committees who help educate other people, especially children, in Water, Sanitation and Hygiene. In Ethiopia, we are working with partners to train teachers in WASH so they can pass on their knowledge to thousands of students. Our work in Ethiopia has also involved fixing up latrines and providing menstrual supplies, both of which can help keep teenaged girls in school longer.
Antibiotics also go a long way to preventing and treating existing cases of trachoma. We work with local governments and partner organizations to provide these antibiotics to areas with high prevalence of trachoma. Earlier this year, we collaborated with partners in a Mass Drug Administration project in Kenya’s Narok County. Despite wet road conditions that made it challenging for crews to access all the communities, the project managed to administer the antibiotic azithromycin to more than 215,000 people!
Throughout the process, our trained community health volunteers work tirelessly to provide education on the importance of facial cleanliness and environmental improvements in stopping the spread of trachoma.
Finally, with help from our generous donors, our partner hospitals can offer surgeries free of charge to people with advanced stages of trichiasis to alleviate the pain and prevent further loss of sight.
We’re involved in clean water projects as a means of preventing trachoma, but the effects of providing clean water to communities are countless. The installation and maintenance of boreholes prevents dozens of waterborne diseases that sicken and threaten the lives of many, and that keep whole communities trapped in the cycle of poverty. Sustainable boreholes help people grow gardens full of fresh vegetables, allow them to raise livestock and improve the quality of life for everyone around them.
The effects of access to clean water are especially beneficial to women and girls. Here’s why:
Education and economic opportunities: In many communities, women and girls are responsible for fetching water, a task that can be extremely time consuming and physically demanding. This can prevent girls from attending school and women from pursuing income-generating activities. When clean water is locally available, girls are more likely to complete their schooling, and women have more time for activities that empower them economically.

Reduced gender-based violence: Providing access to clean water within communities reduces the need for women and girls to travel long distances for water, decreasing their vulnerability to the violence and harassment that they risk when collecting water.
Hygiene and menstrual health: Clean water is essential for maintaining proper hygiene, including menstrual sanitation. When women have access to clean water and sanitation facilities, it positively affects their overall health and dignity.
Community development: Women are often key contributors to the well-being of their communities. When they have access to clean water, they can actively take part in and lead initiatives that enhance the overall living conditions in their communities.
In 2023, we partnered on two new boreholes at schools in Ethiopia’s Amhara Region. In Zambia, we repaired 25 boreholes in the Mkushi District, trained 20 new Area Pump Minders and set up more WASH committees.
You can help us continue our water projects in 2024 by making a donation today. Thank you for your support!

At 32, Stephen is the proud father to four children in Narok County, Kenya. But providing for his family has been challenging for the young dad. Since high school, he’s been struggling with painful, tearing and itchy eyes.
Stephen started out raising livestock but found it difficult to make ends meet. He then tried more lucrative work as a motorcycle taxi driver and courier, but his poor eyesight combined with the dusty country roads made the job too dangerous for him.
Eventually, Stephen visited a private hospital where he was diagnosed with trachoma, an infectious eye disease that causes the eyelid to turn inward. As a result of the disease, the eyelashes rub against the eye, causing intense pain, scarring of the cornea and, if left untreated, blindness.
Stephen received a pair of eyeglasses at the hospital and was sent on his way, but he found that the glasses only made things worse. By this point, his right eyelid was so swollen that it was starting to obscure his vision and caused his eye to tear up constantly.
Stephen went to another hospital, where he learned that he needed surgery to treat the trachoma infection in his right eye. With help from his family, Stephen raised the money he needed and got the procedure done. But there was no improvement to his eyesight, and before long, the trachoma infection had returned.
Many villagers are happy about this project because it has literally opened their eyes.”
With remarkable doggedness, Stephen went to a third hospital. Again, he underwent surgery. And again, his condition didn’t improve.
After that, Stephen nearly gave up. But then something happened to reignite hope. He finally crossed paths with Operation Eyesight.
In October, Stephen heard that there would be free eye camp for trachoma patients at the Ntulele Health Centre on World Sight Day, which falls on the 12th of the month. He visited the centre to learn more, and a surgeon examined him and recommended another operation. Stephen recounted his previous experiences, but the surgeon reassured him that they could improve his condition.
Stephen returned to the health centre later in October, and along with many others, underwent his third procedure. Thanks to the generous support of our donors, Stephen got the surgery done free of charge. After the bandages came off, he was filled with joy and relief. His vision was unobscured once again. His right eyelid had been surgically rotated back into place, and his cornea had been spared of any scarring.

“Now I can get back to my motorcycle business,” he says, “just like the other young men from my village.”
Stephen adds that he is grateful for the work Operation Eyesight is doing in his village through the eye health outreach programs.
“Many villagers are happy about this project because it has literally opened their eyes,” he says. “A lot of people had eye problems, but now they have been treated.”
As well as resuming his work to support his family, Stephen is also acting as an eye health ambassador in his village. When community health workers who work in the village encounter a patient who is nervous about getting surgery for their trachoma, they call on Stephen to share his experience.
With files from Eunice Mwihaki Murigi.
Did you know trachoma is the leading cause of preventable blindness in Kenya and many parts of Africa?
This painful bacterial infection causes irreversible blindness if left untreated. Worse yet, women and children are more likely to contract this condition.
We are supporting the distribution of antibiotics in Kenya’s Narok County to treat and reduce transmission of trachoma. This is happening in partnership with the local Ministry of Health and other partners, with the goal of eliminating trachoma from the county by 2025.

“Narok is home to many who raise cattle, which attracts flies that spread trachoma. We are now building on the success of our work to date in the area,” explains Alice Mwangi, our Country Director for Kenya. “Treating and preventing transmission of trachoma through distribution of antibiotics is one of the most effective ways to eliminate this condition from entire regions.”
In 2021, our Kenya team distributed antibiotics to more than 460,000 people in Narok, covering nearly 90 per cent of the target population for this program. In summer 2022, we are leading another planned Mass Drug Administration (MDA) in the region.
Our trachoma elimination projects are designed to implement all four components of the World Health Organization-recommended SAFE strategy:
• Surgery to treat advanced cases of trachoma;
• Antibiotics to eliminate infection, which includes Mass Drug Administrations (MDA);
• Facial cleanliness; and
• Environmental improvement such as wells, boreholes and latrines.
In the village of Kwanga, in southern Zambia, the rehabilitation of a borehole has meant local access to abundant, fresh water for the entire community.
For Natasha, it’s brought the ability to attend school full time. Previously, she had to walk several kilometres each day to fetch water for her family. This took so much extra time and energy that she began missing school.
Together, we rehabilitated Kwanga’s borehole in 2021. It’s one of 96 non-functioning boreholes that we have rehabilitated in the past three years, in addition to the 106 that we have drilled in the Sinazongwe district, in Zambia’s arid south.
This has helped eliminate blinding trachoma infections from the district. Locally-available water has also brought a host of benefits across communities like Natasha’s, including improved health outcomes, thriving local economies and improved opportunities for women and girls.
"Access to fresh water prevents the spread of trachoma and other infections and also brings many benefits to the local community,” explains Vikas Gora, our Global Director of International Programs.

Now that the borehole in her village is functioning again, Natasha and several other girls in her class no longer have to haul water for long distances, and they are back attending school full time.
Access to clean water doesn’t just help reduce the spread of infection — it brings long-lasting and sustainable change to the entire community.
Thanks to our donors and partnerships with local Water, Sanitation and Hygiene (WASH) committees that are trained to maintain boreholes and ensure their longevity, we’re creating a ripple effect that is being felt in other communities across Zambia.
When Elina started to experience agonizing pain in her eyes, her options were limited. She lived in Munkala village in Zambia, more than 120 km away from a hospital, and her family couldn’t afford to travel there for her to see a doctor. They spent all they had looking for answers from traditional healers nearby, but Elina continued to suffer.
When Elina was discovered by Operation Eyesight, she was diagnosed with trachoma, a bacterial disease that leads to permanent blindness if it isn’t treated. Fortunately, she was diagnosed before she lost her vision. The surgery to treat her in-turning eyelashes and antibiotics to treat the infection were provided free of charge, thanks to our generous donors.
The following year, Elina’s vision had worsened, and she was diagnosed with cataracts. Once again, our donors made it possible for Elina to have surgery, this time to restore her vision.
Operation Eyesight’s mission is to prevent blindness and restore sight, and through support from our donors and partners, we were able to prevent blindness due to trachoma, and restore sight lost through cataracts for Elina. She now lives without pain, and she’s able to contribute to her family by cooking meals and walking to the nearby borehole to fetch clean water. Her life has been transformed, and she is smiling once again.

Regina is a 36-year-old mother of five who lives in Zambia’s Sinazongwe district. To provide her family with clean water, she visited her village’s borehole every day until 2018, when the borehole became dysfunctional and stopped providing clean water. At that point, the next closest borehole was 10 kilometres away.
In communities like Regina’s, providing water is generally the responsibility of the women and children of the household. With such a long distance to travel to collect clean water, they were unable to do anything else, including attending school.
When they didn’t have enough clean water, they were forced to collect from unclean sources, and Regina’s household usually suffered from diarrheal diseases. They also faced the risk of contracting trachoma, a painful bacterial disease that can lead to permanent blindness. All this sickness and daily walking took its toll on Regina and her children, and it interfered with her children’s ability to get an education.
In 2020, Operation Eyesight rehabilitated the borehole in Regina’s village, transforming the lives of her and her children. Thanks to donor support of our borehole programs, Regina is able to collect clean water right in her own community. Her children are healthier and can attend school, and she has time to do other things, including working in her vegetable garden.
This Mother’s Day, you can help a mother like Regina provide clean water for her family. Please donate to Operation Eyesight to help prevent blindness and restore sight for women and girls. Every dollar will be used to ensure they get the quality eye health care they need right now, and well into the future. You can choose to make a donation in the name of your own grandmother or mother or another important woman in your life.
This year’s World Water Day theme is valuing water. On March 22, we celebrate World Water Day by recognizing that the value of water is much more than its price. Water is an integral part of our daily lives and impacts health, education, economics and our environment. Ensuring the availability and sustainable management of water and sanitation for all is listed by the United Nations as one of their 2030 Sustainable Development Goals. Clean water is also incredibly valuable in eye health.
Access to clean water is an important part of ending serious eye infections like trachoma, the world's leading cause of preventable blindness. Trachoma causes the eyelid to turn inward so that the eyelashes rub the eyeball. This results in intense pain, scarring of the cornea and ultimately, irreversible blindness. Although trachoma can be treated with medicine and, in more severe cases, surgery, the most effective way of reducing rates of this painful infection is to address one of the root causes, which is lack of adequate sanitation. With access to clean water, people can wash their hands, faces, clothing and homes and prevent the spread of trachoma. This improved sanitation also aids in the reduction of other serious illnesses such as diarrheal disease, upper-respiratory infections and other communicable diseases like COVID-19.

Operation Eyesight follows the World Health Organization-endorsed SAFE strategy for eliminating trachoma in areas of Kenya and Zambia. SAFE is a comprehensive treatment and prevention program that includes:
Properly implemented, the SAFE strategy permanently eliminates trachoma. One of the key factors for achieving this is drilling or rehabilitating boreholes. In recent years, we’ve shifted our focus from drilling new boreholes to rehabilitating existing, dysfunctional boreholes. The cost-savings employed by this method allow us to reach many more communities.

When a borehole is drilled or rehabilitated, we establish local Water, Sanitation and Hygiene (WASH) committees. These committees are trained on how to maintain the borehole and ensure its longevity. Properly maintained boreholes can provide clean water for decades. The WASH committees also provide community health education sessions to help people improve their sanitation habits. They incorporate messages on facial cleanliness and environmental improvements such as the proper building of latrines.
Clean water does so much more than prevent blindness. Families are able to grow more nutritious food and easily water their livestock when water is easily accessible. This leads to a reduced prevalence of illnesses resulting from poor nutrition. It also gives women and girls more opportunities. The task of hauling fresh water for long distances most commonly falls to women and girls. Depending on the area, the journey can also be dangerous, and the water from unprotected sources may not be safe. When clean water is easily accessible, women and girls have time to go to school, earn a living independently, and be actively involved in their families and communities.

Communities with a clean water source also become hubs of local trade and provide increased economic opportunities. New schools are often built near boreholes because of their central location and easy access to water. Existing schools are expanded on to accommodate for the increase in attendance resulting from more girls being able to participate in school now that they don’t have to walk far distances to fetch water. Read this story about how a borehole increased the attendance at Mweela School by 274 students.
This World Water Day, you can help bring the positive ripple effects of clean water to a community in need. Please donate today.